
Ewan Cameron, Ava Helen and Linus Pauling. Glasgow, Scotland, October 1976.
[Part 3 of 4]
By 1970, the year that Linus Pauling published Vitamin C and the Common Cold, the federal government’s “war on cancer” was soon to arrive. The National Cancer Act, passed in 1971, increased federal funding for treatment and prevention research, embracing cytotoxic treatment solutions like chemotherapy. That same year, Pauling began to push for investigations between nutrition and cancer, especially concerning vitamin C. Since the role of vitamin C in immune defense is arguably much less significant than Pauling supposed, the idea that intake of vitamin C should prevent or treat cancer seemed ludicrous to many physicians. Incredibly, evidence is now emerging that the opposite might be true.
In hindsight, there is a tendency for critics to see Pauling simply as a politically liberal proponent of alternative medicine; one who lashed out against a consumerist medical establishment that was firmly supported by conservative citizens, among others. However, proponents of alternative health and holism in the 1960s and 1970s prescribed to a broad range of political ideologies; Pauling was just one among many people who were searching for better preventative and alternative treatments.
In 1980, when Pauling was actively campaigning for a vitamin C treatment for cancer, Americans spent 13.1 billion dollars on cancer diagnosis and treatment. Five years later, a survey of over one-thousand individuals showed that a majority believed clinics using unorthodox cancer therapies should be permitted to operate in the U.S., and just over half said they would seek alternative treatment if seriously ill.
Pauling and his ideological positions are remembered now as having been central to the vitamin C “movement.” Perhaps this is because he was renowned in many arenas and easily attracted a great deal of media attention. Or perhaps, especially knowing his penchant for protesting against nuclear weapons testing and war, this was another issue on which Pauling was the most outspoken opponent of what he saw as a wrong to be made right.
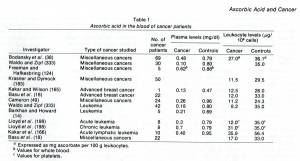
Table from “Ascorbic acid and cancer: a review”, co-authored by Pauling and Cameron, 1979.
For Pauling, the continuing suffering of cancer victims was unnecessary, since a useful treatment was already cheap and readily available. He argued that,
The involvement of ascorbic acid (vitamin C) in the natural defense mechanisms is now known to be so great that we hope that a really significant control of cancer might be achieved by the proper use of ascorbic acid.
Of the studies that Pauling found so convincing, none were as crucial as those conducted at the Vale of Leven Hospital, near Glasgow, Scotland. There, Dr. Ewan Cameron found that mega doses of vitamin C (10 grams daily or more) seemed to slow and even reverse cancerous growth in some patients. He wrote to Pauling in 1971, who eagerly responded that this “attack” on cancer was the most promising application of vitamin C that he knew of. Pauling, who had been studying the role of dietary vitamin C in issues of orthomolecular psychiatry such as schizophrenia, now shifted his focus to cancer.
Far from being the flaky alternative health guru that many came to see him as, Pauling’s work with vitamin C— like all his research on the subject of orthomolecular medicine (a field that he spearheaded)— was consistent with a biomedical model of molecular disease. Since Pauling saw this work as fitting within the framework of molecular biology, it was frequently unclear to him why the medical community resisted what was, to him, a straightforward and significant scientific endeavor.
Further complicating matters was the fact that Stanford University, Pauling’s academic home at the time, rejected his request for additional lab space to pursue cancer research. Now the target of regular media pummelings, Pauling’s ideas were becoming a potential source of bad press for the university. Refusing to take no for an answer, Pauling and his young lab assistant, Arthur Robinson, solicited private funding to continue their work on vitamin C outside of the university setting. Raising $50,000 in donations from wealthy supporters of vitamin therapies, the duo helped to found the Institute for Orthomolecular Medicine in 1973, subsequently renamed the Linus Pauling Institute of Science and Medicine (LPISM) one year later.
From 1973 to 1976, Pauling published co-authored articles with Cameron, who continued to study the effects of vitamin C on cancer from his base in Glasgow. And in 1975, Pauling and Robinson secured additional funds to begin their own animal testing. Two years later, the collaborators began reporting their results in the Institute’s newsletter. In 1979 Cameron and Pauling likewise published an extensive review article in Cancer Research that cited previous studies corroborating their own conclusions. The duo published their book, Cancer and Vitamin C, that same year.

A sample of Pauling’s notes compiled in response to the Mayo Clinic trials, 1979.
Cameron and Pauling’s data seemed to show that vitamin C would be especially valuable for cancer patients. Whereas a daily intake of 10 g of vitamin C in a healthy individual would bring the vitamin C level in the blood to a saturation point that could not be exceeded by increasing or prolonging intake, cancer patients showed a different pattern. Known already to have abnormally low blood levels of vitamin C, the patients in fact achieved just over half the same level of vitamin C blood saturation found in healthy individuals subscribing to a daily intake of 10 grams. For those afflicted with cancer, it was seen as necessary to take 10 grams a day just to reach the normal level of vitamin C found in healthy individuals who did not take supplements at all.
To Pauling, this alone justified continued research on the matter. After persistently stating his case to Dr. Vincent De Vita, director of the National Cancer Institute, two rounds of trials were conducted through the Mayo Clinic to solve what the medical community perceived to be problems in Cameron’s studies. When the trials indeed failed to produce anything like Cameron’s results, funding effectively dried up for vitamin C research – a significant blow to LPISM’s functional well-being.
In response, Pauling and his supporters argued that the Mayo Clinic was missing the point. The Mayo trials had attempted to measure the effectiveness of vitamin C in a manner similar to drug treatments, because the advent of chemotherapy and antibiotics, and the biases of the pharmaceutical industry, had placed primary medical emphasis on the disease, and not on the patient. Pauling saw the results of the Mayo studies not as a definitive defeat, but as the triumph of a complex of interdependent federal and private organizations that held a vested interest in supporting the chemotherapy status quo.
Pauling had claimed that, with vitamin C, lifespan could be increased, tumors could regress, and even full recovery was possible. For many in the medical community, these were not only foolish assertions, they were dangerous as well.
Dr. Charles Moertel, chairman of the Department of Oncology at the Mayo Clinic, was particularly vocal in his rebuke, stating that
For such a message to be conveyed to desperate and dying people, with the endorsement of a Nobel laureate, the presumption must be that it is based on impeccable scientific methodology.
Moertel’s implication, of course, was that Pauling’s argument was instead based on unsound science and certainly lacked the scientific basis to challenge the use of chemotherapy.
Yet vitamin C retained a broad appeal because many saw the prevailing treatment, and its manifold side effects, as inhumane. John Cairn, head of the Mill Hill Laboratory of the British Imperial Cancer Research Fund, provided a voice to the other side the coin by calling out the survivorship data. To wit: in 1986, 200,000 patients were receiving chemotherapy and, by 1991, five year survival rates for colon cancer remained at just 53%. Cairn spoke for many in suggesting that, when it came to the prevailing course of treatment, “the benefit for most categories of patients has yet to be established.”

Ava Helen Pauling, June 1981.
For Pauling, the debate turned from the public to the personal when, at the height of his study of vitamin C, his wife Ava Helen was diagnosed with stomach cancer. Following Ewan Cameron’s advice, she took 10 grams of vitamin C daily, and did not receive chemotherapy. Throughout her treatment, Linus clung to the belief that mega doses of vitamin C would work for Ava Helen, just as it had for Cameron’s success stories in Scotland.
“Daddy was convinced that he was going to save her,” remembered Linus and Ava Helen’s daughter, Linda. “And that was, I think, the only reason he was able to survive… He said to me after she died that until five days before, he thought he was going to be able to save her.”
Ava Helen Pauling passed away in December of 1981. And though he was badly shaken by his wife’s death, belief in the value of vitamin C in the fight against cancer did not fade from Pauling’s mind. Suffice it to say, the medical community remained whole-heartedly unconvinced.
Filed under: Orthomolecular Medicine | Tagged: Ascorbic Acid, Ava Helen Pauling, cancer, Charles Moertel, Ewan Cameron, Linus Pauling, Vincent DeVita, vitamin C |








Leave a comment